Oct 3, 2016 | By Nadia Sheikh
The History of Opioids in America: Pain Patients or Prescription Addictions?
Addiction Resources Painkiller Addiction
How can we prevent overdose deaths from prescription opioids, while still protecting the right to quality healthcare for chronic pain patients? There’s heated controversy surrounding the issue lately.
Despite the rising death toll from prescription opioid overdoses, many patient advocates maintain that no restrictions should be placed on doctors and pain clinics. Some comment that “the drug overdoses are from heroin and other illicit drugs not prescription drugs,” even though, in 2014, there were 18,893 overdose deaths related to prescription painkillers compared to 10,574 overdose deaths related to heroin.
Others argue that these people are ‘patients,’ not ‘addicts.’ A line is being drawn between the two, denying the reality that some patients are or become addicted to prescription painkillers. Addiction doesn’t discriminate, and often isn’t a matter of choice. It’s very possible to develop a physical dependence on opioids over time, which can lead to addiction.
The dangers of addiction were apparent early in the history of opioid painkillers in America. But, the 1980s saw a crucial turning point in American medicine, which has contributed to the immense scope of abuse we see in today’s opioid epidemic.
At First, Opioids Changed the Medical World
The history of opioids’ medical use traces back to 3400 B.C., when the Sumerians in lower Mesopotamia were cultivating the opium poppy, known as “Hul Gil”—the “Joy Plant.” Opium was used by many ancient cultures—the Assyrians, Egyptians, Arabs, Greeks, Romans, and Chinese.
By 1527, the Swiss-German alchemist Paracelus had introduced the use of opium pills in medicine. Finally, in 1806, German chemist Friedrich Wilhelm Adam Sertürner isolated morphine from opium, named after the Ancient Greek “god of dreams,” Morpheus.
Morphine became a mainstay in U.S. medical treatment throughout the 19th century for pain, anxiety, respiratory problems, “consumption,” “women’s ailments.”
But Their Danger Is Old News
By the end of the Civil War, so many soldiers were hooked on morphine that the addiction became known as “Soldier’s Disease.” Heroin was then synthesized in 1898, and Bayer offered it as a cough suppressant and “non-addictive” morphine substitute for medical use. But, the dangers of opioids were becoming increasingly known.
In 1914, the Harrison Narcotics Tax Act essentially prohibited prescription opioids by making it extremely difficult for doctors and pharmacists to distribute the drugs. Because of its hazards and high risk for dependence, Bayer stopped mass production of heroin and The Heroin Act made the drug illegal even for medical use in 1924.
The medical community still remained conflicted about the safety of opioids. By many, morphine was considered a substitute for alcoholics, and “morphinism” itself was seen as a disease—“in the majority of cases, initiated, sustained and left uncured by members of the medical profession.”
So, What Changed?
Trying to maintain the painkilling effects of morphine and heroin but lessen the risk of dependence, in 1916 German scientists synthesized a new wonder drug—oxycodone. After WWII, “nerve block clinics” were opened in the ‘50s to treat injured soldiers’ pain without resorting to surgery. Since the ‘60s, oxycodone abuse has been a consistent problem in the U.S.
Medical professionals remained fearful of prescribing opioid drugs. But, the World Health Organization (WHO) had endorsed the medical use of morphine in 1969, because it “doesn’t inevitably lead to dependence.” They made a dangerous distinction between physical dependence and “drug dependence”—which they defined by “difficulty controlling consumption, compulsive use, and inappropriate social behaviors.”
In 1980, Dr. Hershel Jick published a famous letter that changed American medicine, stating, “the development of addiction is rare in medical patients with no history of addiction.” Then, Dr. Russell Portenoy deemed opioids the “safe, salutary and more humane” treatment for chronic pain, based on “opioid maintenance therapy” used for his non-cancer patients.
Pain Treatment Was the New Priority
‘Humane’ pain treatment became a priority in the ‘90s for all pain types. New opioids started coming on the market with extended-release formulas—like OxyContin in 1996.
Purdue Pharma, the makers of OxyContin, promoted it as a miracle drug for chronic pain patients. In their 1997 marketing video, a doctor says “they don’t wear out; they go on working; they do not have serious medical side effects,” and that they “should be used much more than they are for patients in pain.”
Soon after, opioid prescriptions skyrocketed by the millions. Organizations began to advocate for medical standards that required doctors to conduct pain assessments with all patients.
The Ugly Truth Begins to Surface
Purdue Pharma pleaded guilty to misleading the public about Oxycontin’s addictive nature in 2007, and settled with the government for $635 million. In 2010, they released an abuse-deterrent version of OxyContin, which made it harder to crush and dissolve the drug.
In a medical survey on the new drug formula, though abuse of OxyContin decreased, 24% of people found a way around the abuse-deterrent properties and 66% switched to other opioids. Many people in the study “moved on to heroin [because] it is easier to use, much cheaper and easily available.”
By 2002, opioid analgesic poisoning was listed as cause of death more commonly than heroin or cocaine. By 2010, overdose deaths due to prescription opioid pain relievers had more than tripled in 20 years, causing 16,651 deaths in the U.S. As their addictive reality came to light, even old opioid advocates admitted where they were wrong.
In 2011, Dr. Portenoy admitted that he and his team “often left evidence behind,” as his goal back in the ‘80s was to de-stigmatize opioid drugs. In light of the epidemic caused by opioids in America, he said: “Clearly if I had an inkling of what I know now then, I wouldn’t have spoken in the way that I spoke. It was clearly the wrong thing to do.”
Scope of Opioid Abuse Today
Much like the early history of heroin in medicine, prescription opioids are now coming under increasing scrutiny for their dangerous, adverse effects. Many people suffer from a Substance Use Disorder (SUD) with prescription pain relievers, in which their recurrent use of the drugs “causes clinically significant impairment, including health problems, disability, and failure to meet major responsibilities at work, school, or home.”
Opioids are frequently used ‘nonmedically,’ which means using a drug without a prescription of your own—or simply for the feeling the drug produces. In the U.S. today, opioid painkillers are the most abused prescription medication:
- 227 million opioid prescriptions were written in the U.S. in 2015.
- By 2011, there were 5 times more more treatment admissions for prescription pain relievers than in 2001.
- In 2014, 3 million people were nonmedical users of pain relievers.
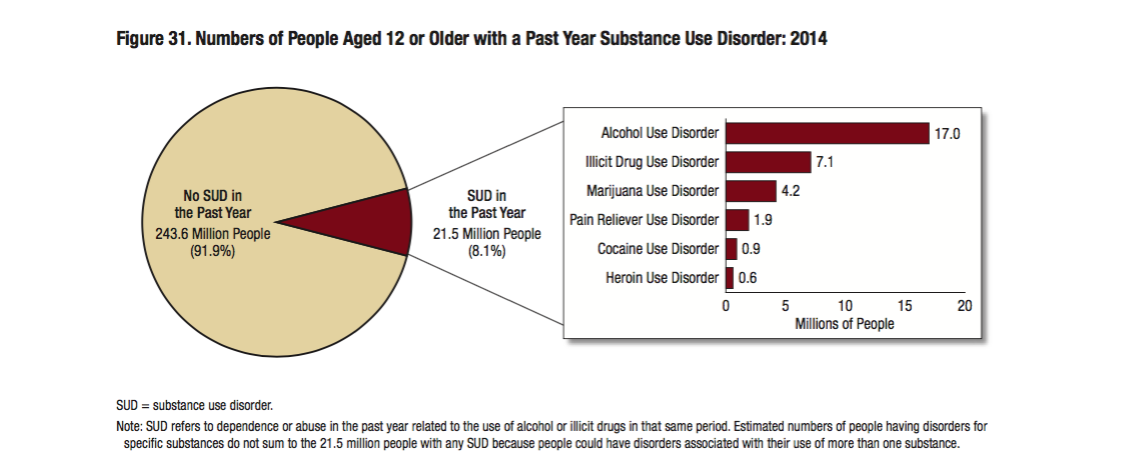
- Of the 5 million people in the U.S. with a Substance Use Disorder (SUD) in 2014, 1.9 million had a pain reliever use disorder, while 0.6 million people had a heroin use disorder.
Both heroin and prescription painkillers act upon the same brain systems. Because of this, prescription opioids also “present an intrinsic abuse and addiction liability,” according to Dr. Nora Volkow, the Director of the National Institute on Drug Abuse (NIDA).
These drugs are most dangerous when used for non-medical purposes. But, some people are prescribed these medications and still increase their risk for addiction (or even overdose) by not taking take them as prescribed—taking more pills at once, taking them more frequently, or combining them with other medications.
Dr. Volkow also acknowledges that “it is possible for a small number of people to become addicted even when they take them as prescribed, but the extent to which this happens currently is not known.”
Patients or Addicts?
In the U.S., there are around 100 million people suffering from chronic pain—most commonly moderate-to-severe back pain conditions and osteoarthritis. For some patients, long-term opioid treatment has provided relief without jeopardizing their quality of life. But, other patients start to need higher doses to numb their pain, which can lead to dependence and addiction.
There’s little data to support the benefits of opioids, but there is some evidence of their harm and addiction potential. One study found that, among people who were treated with opioids for 3 months, 50% were still using the painkillers 5 years later. Among 39 existing research studies, up to 26% of patients developed a physical dependence.
As evidence of this dependence, research also suggests there’s a relationship between opioid painkillers and abuse of heroin—the prescription drugs’ illegal cousin. According to NIDA, three recent studies show that nearly half of young people who inject heroin say they abused prescription opioids before starting to use heroin, and some took up heroin because it’s cheaper and easier to get.
It’s clear that opioid drugs can take a powerful hold on both nonmedical users and patients. Whether we call it addiction, dependence, or reliance, we need to be prepared for it.
A Brighter Future
As opioid dependence and overdose deaths remain at crisis levels, we need forward-thinking solutions:
- More research about benefits and risks of long-term opioid treatment.
- Maximize the use of non-medication strategies for pain management.
- Explore new, non-opioid medications.
- Develop screening tools to assess a patient’s potential for medication abuse
- Create adequate resources to help people who develop a dependence.
Above all, we need to remain open-minded and move beyond a one-dimensional view of addiction. Whether a patient or non-medical user, when opioid dependence develops, the door to asking for help needs to be open.