Aug 29, 2016 | By Nadia Sheikh
What Form of Treatment is Proven to Be the Most Effective?
Addiction Resources Addiction Treatment Aftercare and Sober Living Inpatient Addiction Treatment Recovery
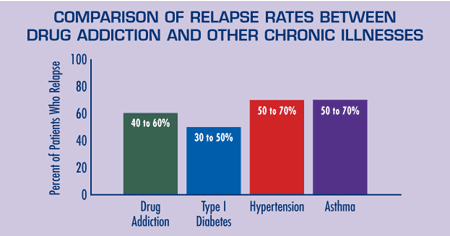
Like other chronic illnesses, relapse rates for addiction are high—ranging from 40-60%. Relapse by no means signifies that treatment has failed, but is there a form of treatment that’s proven most effective?
The National Institute on Drug Abuse (NIDA) is dedicated to advancing scientific knowledge about addiction, in order to improve treatment outcomes. They’ve established that effective addiction treatment must help an addict:
- stop using drugs and/or alcohol.
- stay sober.
- be productive in their family, at work, and in society.
Addiction is a unique condition—there’s no universal, one-size-fits-all treatment method. But, there’s a growing understanding of what makes addiction treatment more effective.
Uses Research-Validated Techniques
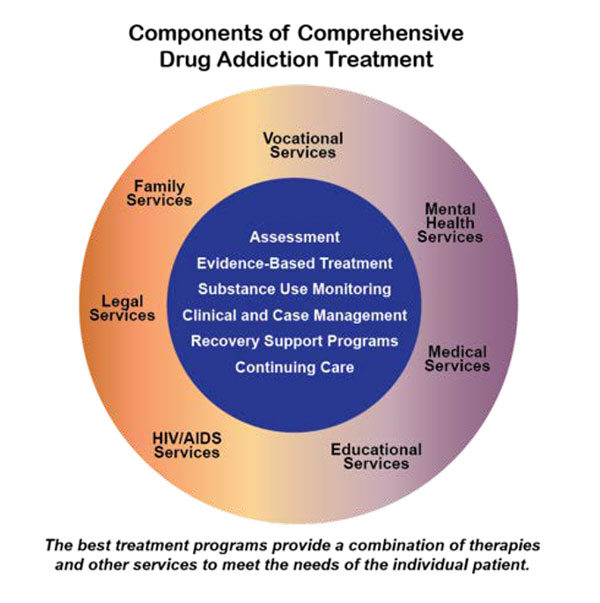
NIDA has defined several components of comprehensive treatment, one of which is the use of techniques that are validated by research. All health care systems are built on evidence-based practices, to establish the most effective methods of care. Yet, addiction treatment has lacked national, evidence-based standards concerning who can provide treatment, core competencies for those providers, and facility regulations.
Because of its complexity and misplaced stigmas on the condition, addiction treatment has been separated from mainstream medicine for a long time. Now, the two are starting to merge, but there’s a gap between emerging research and older treatment approaches. It’s difficult for professionals to come to a consensus.
Traditional treatment approaches are derived from multidisciplinary treatment of chronic mental disease and the peer-support program of Alcoholics Anonymous, founded in 1935. The 12 steps help countless people address psychological and spiritual aspects of their addictions, and are widely-accepted within the treatment community. There are physicians, too, who believe in the effectiveness of AA.
The research on the matter is varied—some studies confirm AA’s effectiveness in treating addiction, while others say there’s no experimental evidence to support it. Some 12-step advocates worry that new scientific research will make 12-step recovery a “dying art.”
There are now ongoing scientific investigations, establishing evidence-based practices for addiction treatment. Yet, in a 5-year study, the National Center on Addiction and Substance Abuse (CASA) at Columbia University found that “only a small fraction of individuals receive interventions or treatment consistent with scientific knowledge about what works.”
The evidence is still building, slowly being integrated with traditional methods like 12-step recovery. Most importantly, few evidence-based practices in addiction treatment are deemed universally effective—they vary for each individual, their situation, and their substance of abuse. Making treatment more effective means synthesizing newer scientific evidence and older practical knowledge to provide options—to find what works for each individual.
Clinical Expertise
In the same CASA study, they found one, glaring problem: insufficient care. Most medical professionals are not sufficiently trained to diagnose or treat addiction. Most addiction treatment providers aren’t well-equipped to provide the full range of effective treatments—lacking the scientific knowledge, proper skills, and medical credentials.
Researchers from UCLA determined clinical expertise is the essential criterion that improves treatment outcomes universally. In a review of current evidence-based practices, researchers found that effectiveness varies in different situations, but clinical expertise is key to making any treatment practice more effective.
Without clinical expertise, evidence-based practices can’t be properly implemented. Physicians should be certified by the American Board of Addiction Medicine. A study by the Clinical Trials Network found that counselors and therapists with higher-education degrees were more capable of applying evidence-based practices. For the best outcomes, addiction treatment professionals need adequate education and training.
Therapy and Resources for Underlying Problems
According to NIDA, “to be effective, treatment must address the individual’s drug abuse and any associated medical, psychological, social, vocational, and legal problems.”
Substance abuse has different roots for everyone. Co-occurring mental illness plays a role in addiction for many people—about one third of all alcohol abusers and more than half of all drug abusers. Effective treatment involves licensed clinicians with the expertise necessary to assess and treat underlying mental health conditions, as well as behavioral disorders. There must be one-on-one attention and access to medications if needed.
In her book “Inside Rehab,” science writer Anne M. Fletcher talks about the contrast between scientifically-validated methods and actual practices in treatment. She says, “Treatment should be individualized. One size does not fit all.” Substance abuse can involve a variety of underlying problems—unresolved emotional conflicts, chronic pain, infectious diseases, family conflicts, and legal or employment issues. Effective treatment provides therapy and resources to address issues comprehensively, so addicts aren’t left to face them on their own.
Cognitive-Behavioral Therapy
There are countless forms of psychotherapy, but behavioral therapies are noted among NIDA’s principles of effective treatment. In particular, cognitive-behavioral therapy (CBT) is a widespread, research-validated technique.
CBT focuses on addicts’ thought patterns, how they affect behavior, and learning healthier coping mechanisms. Research on CBT shows it’s one of the most useful treatment therapies because its effects are durable over time. However, some forms of CBT are more effective than others.
As per a review by the Psychiatric Clinics of North America, one of the most effective CBT therapies is contingency management—providing positive reinforcement and tangible rewards for staying sober. Often, aftercare programs offer monetary rewards or additional privileges for clients who pass drug tests, achieve recovery milestones, or participate in recovery activities.
Family and couples therapy are also proven to have significant, positive effects. Addiction has a social component. These therapies incorporate an addict’s home environment into their recovery and help establish a support system.
Though relapse prevention is one of the most popular CBT therapies, existing research shows it has a relatively small effect in the long run. Results from reviews and studies like these help to establish what’s working best. But, despite measures of “small” or “great” effectiveness, many CBT methods have shown some effectiveness in helping people.
Relapse-Prevention Medication
NIDA lists medications among its principles for effective treatment—for safe detoxification as well as co-occurring conditions. There are also relapse-prevention medications, which can decrease cravings and help re-establish normal brain function. Science has revealed that addiction alters brain function by damaging the reward center, creating cravings, and increasing compulsive behavior.
There are approved medications that help opiate, opioid, tobacco, and alcohol addicts remain abstinent from their substance of addiction. Scientists are working on medications for stimulant and cannabis addictions.“ We have some pretty good drugs to help people with addiction problems, but doctors don’t know how to use them,” says Dr. Mark Willenbring, a former director of research at the National Institute for Alcohol Abuse and Alcoholism.
There’s great debate about these medications. Some people become reliant upon them, and there’s a risk that people might see them as addiction “cures.” But, relapse-prevention medications are intended for use alongside other treatment methods—not to be quick-fixes. They can help people with specific cravings, but they don’t ensure complete sobriety.
Harvard Health reminds us: “The most important lesson of all in recent discoveries may be that addictions are chronic conditions for which there are treatments but rarely simple cures.” The reality is, we still need more research. There’s evidence that these medications have helped many individuals struggling with addictions, but the research is not conclusive enough to establish them as an evidence-based practice yet.
Continuous and Long-Term
Detoxification alone does little for long-term change. Research shows that the best outcomes occur with longer durations in treatment—at least 3 months—and long-term care plans. Long-term progress assessments and continuing treatment-plan modifications result in greater success rates. With progressive stages of rehabilitation, addicts are held accountable and treatment plans can be shaped to meet their specific needs.
Anne M. Fletcher notes that most people complete a 30-day program in rehab, yet “people with serious substance abuse disorders commonly require care for months or even years.” A short-term fix isn’t enough.
Treatment and medical professionals alike now accept that addiction is a chronic illness. In the words of Dr. Willenbring: “People with a chronic form of addiction need multimodal treatment that is individualized and offered continuously or intermittently for as long as they need it.”
An Individualized Treatment Plan
The crucial principle of effective treatment is, “No single treatment is appropriate for everyone.” Proper treatment depends on the type of drug that’s abused and a patient’s characteristics. “Matching treatment settings, interventions, and services to an individual’s particular problems and needs is critical to his or her ultimate success.” Ethical medical practice means meeting a patient’s needs, respecting existing scientific evidence, and providing the best care.
Part of treatment’s effectiveness also hinges on the individual’s ability to incorporate what they learn into their life after treatment. It’s important to consider an individual’s values, and “that treatment be appropriate to the individual’s age, gender, ethnicity, and culture.” Research shows the one-size-fits-all approach does not work.
“Novelty seekers and risk takers with insufficient inhibition and judgment will not necessarily respond to the same methods that work for people afflicted by traumatic stress or hypersensitivity to everyday stress,” says Harvard Health. “Treatment will always depend on the type of addiction and the type of addict.”
There are discrepancies between traditional methods and scientific evidence because different things work for different people. One person thrives in a 12-step program, while another thrives with relapse-prevention medication, while another thrives in therapy for a co-occurring condition. Most often, effective treatment involves numerous approaches in conjunction.
Addiction does not discriminate—it affects people from all walks of life. Methodologies must be flexible and capable of meeting a wide range of needs.
Suzan Halterman
8 years ago
Thanks for sharing. I really like how you said that clinical expertise is the essential criterion that improves treatment outcomes universally. I have a cousin that could really use some help with learning how to be sober. I will have to point him in this direction.
recoverycnt
7 years ago
Thanks for sharing. I really like how you said that clinical expertise is the essential criterion that improves treatment outcomes universally. We are addiction treatment specialist from New Jersey
Christine Weeks
5 years ago
Thank you for sharing this content. This is great and appeals to current situation.
Recent Articles
Warning Signs of a Drug Relapse: Spot Them Early
How to Quit Cocaine: Overcoming Addiction & Withdrawal Symptoms
Non 12 Step Fellowships for Flexible Recovery
What are 12-Step Programs? Explore Their Principles and Impact?
What is Relapse? Understanding Recovery’s Twists and Turns?
Question About Treatment
Get Confidential help 24/7
(866) 207-7436Who Answers
Contact Sober Nation's Sponsored Hotline
If you are seeking drug and alcohol related addiction rehab for yourself or a loved one, the SoberNation.com hotline is a confidential and convenient solution.
Calls to any general hotline (non-facility) will be answered by Treatment Addiction Solutions
Alternatives to finding addiction treatment or learning about substance:
If you wish to contact a specific rehab facility then find a specific rehab facility using our treatment locator page or visit SAMHSA.gov.
To learn more about how Sober Nation operates, please contact us